Confronting Entrenched Disparities
Health outcomes in the UK are deeply divided by social and racial lines, with Liverpool ranking as the third most deprived local authority in the country. In this region, residents face a healthy life expectancy of just 58 years, and approximately 30% of children under 16 live in poverty.
Beyond local data, national statistics reveal systemic inequities: Black women are four to five times more likely to die in childbirth than white women, and Black individuals are four times more likely to be detained under the Mental Health Act.
This means there is a critical need to equip healthcare professionals with the tools to recognise and dismantle these avoidable, unfair systemic differences.
SO Health were commissioned by the NHS to enhance healthcare professionals’ insight into the impact of social and systemic disparities.
Empowering Change-Makers
The primary objective was to deepen healthcare practitioners’ understanding of how social and racial inequalities (such as structural racism, socioeconomic disparities, and implicit bias) impact patient outcomes.
The session aimed to:
- Identify key Social Determinants of Health (e.g., housing, education, and income).
- Interpret local life expectancy and health data to understand community-specific disparities.
- Apply the Core20PLUS5 framework, which targets the most deprived 20% of the population and five key clinical areas: Maternity, Early Cancer
- Diagnosis, Severe Mental Illness, Chronic Respiratory Disease, and Hypertension Case-Finding.
- Reflect on personal and systemic biases to foster more equitable healthcare practices.
An Interactive and Reflective Workshop
SO Health delivered a comprehensive training session that blended hard data with personal reflection and practical application. Key actions included:
- Data-Driven Awareness: Facilitating a “Stat Attack” using local Liverpool data to explore the “postcode lottery,” such as the 12-year life expectancy gap between North and South Liverpool.
- Person-Centered Learning: Utilising “Health Inequality Walk Personas”, including an elderly refugee and a young Black man, to help participants visualize how barriers like language and discrimination manifest in real-world scenarios.
- Framework Implementation: Guiding participants through the Core20PLUS5 approach to brainstorm specific strategies for “PLUS” groups, such as inclusion health groups (homelessness, migrants) and those with learning disabilities.
- Skill Building: Conducting role-play exercises to practice responding to common challenges, such as a colleague dismissing health inequalities or navigating language barriers without an interpreter.
The Outcome: Measurable Impact and Improved Confidence
The session results indicate a significant shift in participant awareness and readiness to implement equitable care:
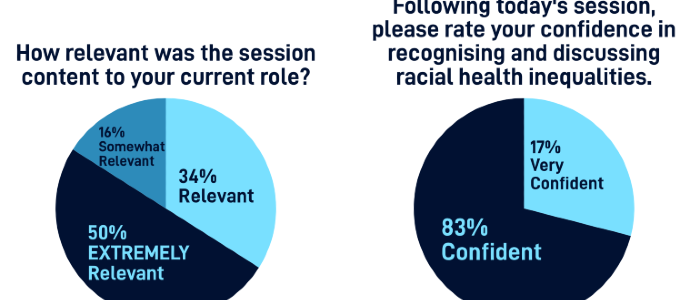
- Knowledge & Awareness: 100% of participants reported that the session deepened their understanding of social and racial inequalities.
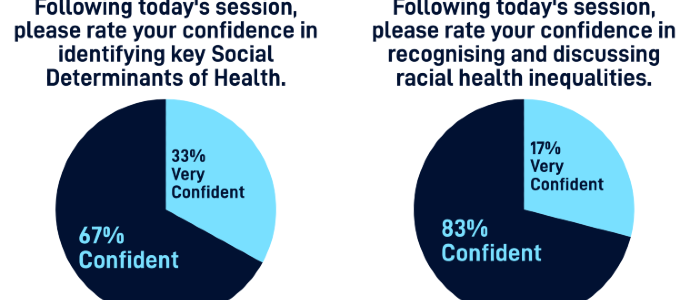
- Professional Confidence: Post-session confidence was high across all core areas. Notably, 100% of participants felt confident in reflecting on personal/systemic biases to support equitable care. Furthermore, 100% felt confident in identifying Social Determinants of Health, and 100% felt confident in recognising and discussing racial health inequalities.
- Practical Application: Participants showed strong readiness to use the Core20PLUS5 approach, with 50% feeling confident as they begin implementation.
- Long-Term Commitment: 100% of attendees stated they are likely or very likely to apply what they learned in their day-to-day practice.
Trainer Excellence: The session was highly regarded, with 100% of respondents finding the trainers positive and effective.